
The Skinny on Hyaluronic Acid: Not Just for Your Face, But Your Knees Too!
By Soundarya Sitaram
9 min to read
Let’s talk about hyaluronic acid (HA). You’ve probably heard of it as the holy grail of skincare—the ingredient behind plump, hydrated, glowing skin. But here’s something most people don’t realize: this same molecule plays a critical role inside your joints.
Yes—your knees rely on it just as much as your skin does. And when it starts to break down, you don’t just lose “glow”— you lose comfort, movement, and quality of life. So let’s break it down—simply, clearly, and with a bit of perspective
HYALURONIC ACID: MORE THAN JUST A PRETTY FACE
And if you’ve experienced knee pain, stiffness, or reduced mobility— this difference becomes very real.
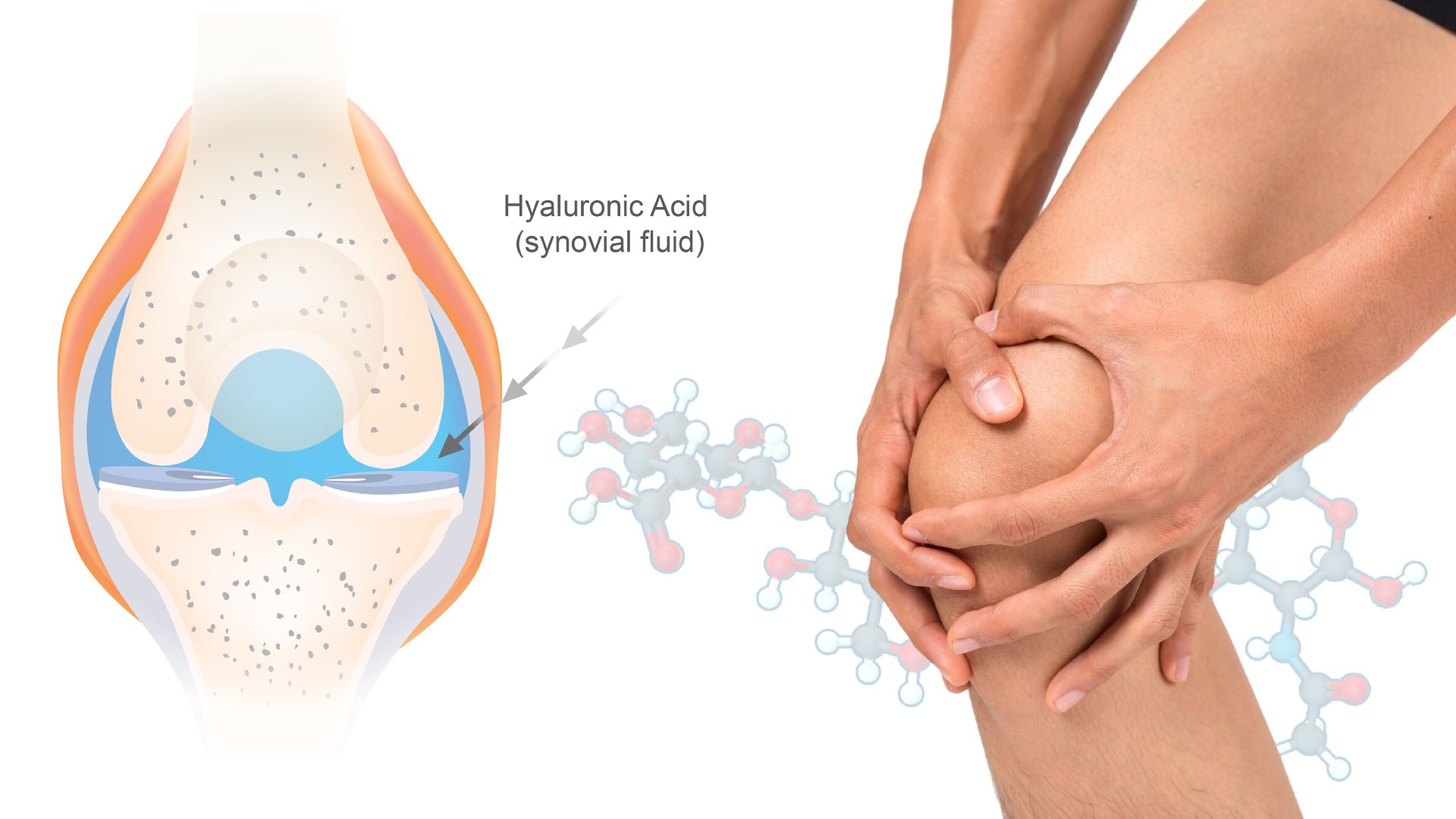
WHAT EXACTLY IS HYALURONIC ACID?
Hyaluronic acid is a naturally occurring molecule in your body.
It’s a gel-like substance with an exceptional ability to retain water—up to 1,000 times its weight.
In your joints, it forms a key component of synovial fluid, which:
➤ Lubricates movement
➤ Absorbs shock
➤ Maintains smooth joint function
When present in the right form, it allows your joints to move effortlessly.
When it degrades, movement becomes restricted and painful.
SKIN HA VS KNEE HA: SAME NAME, DIFFERENT JOB
It’s easy to assume HA works the same everywhere—but it doesn’t.
Feature | Skin HA | Joint HA |
|---|---|---|
Function | Hydration & plumpness | Lubrication & shock absorption |
Structure | Lightweight | High molecular weight, viscous |
Delivery | Topical | Intra-articular (injection |
In joints, HA needs to be stronger, denser, and more functional. This isn’t skincare—it’s biomechanics.
WHAT HAPPENS IN KNEE OSTEOARTHRITIS?
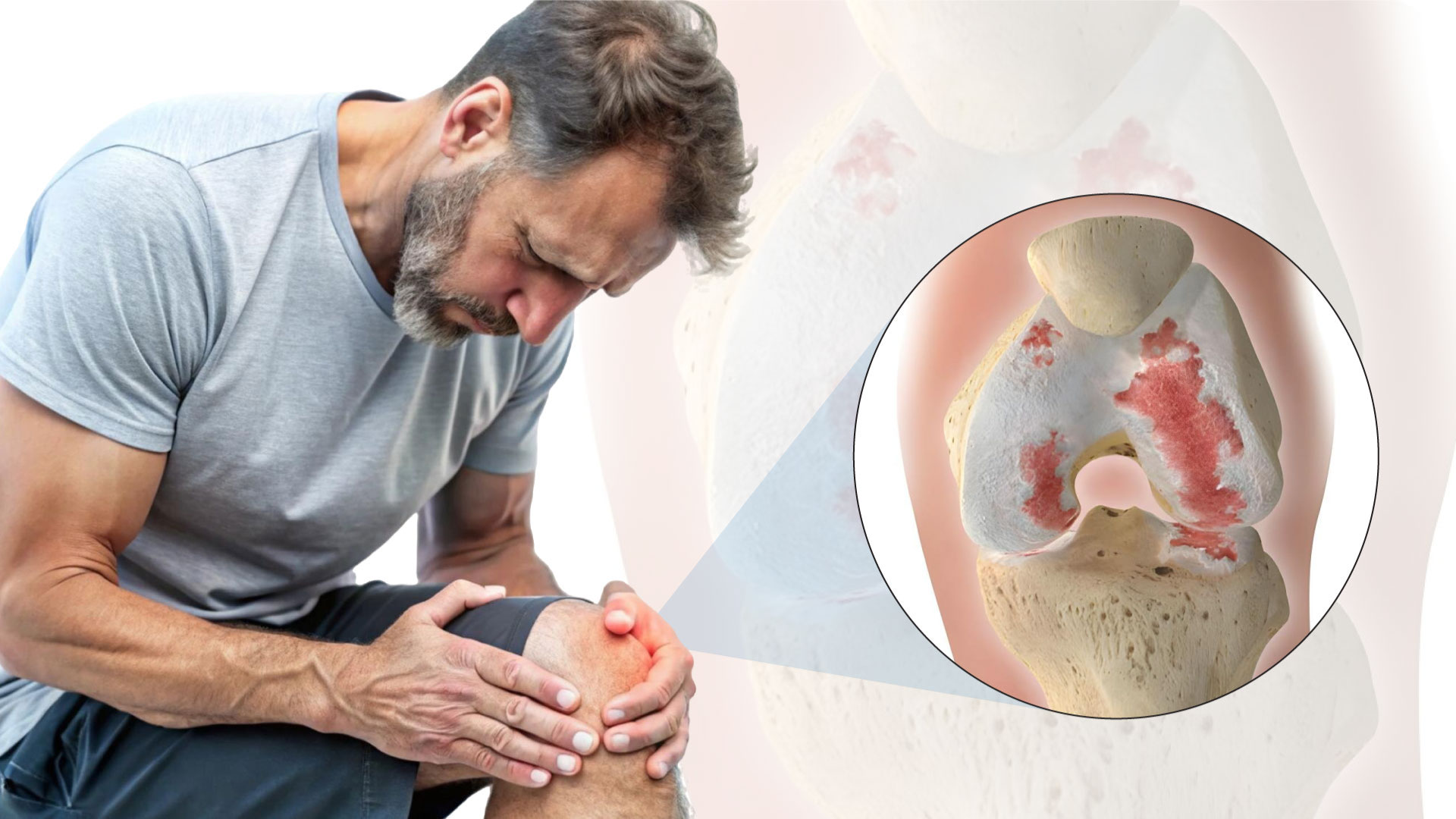
Osteoarthritis doesn’t just affect cartilage—it disrupts the entire joint environment.
Over time:
➤ HA breaks down
➤ Molecular weight reduces
➤ Synovial fluid loses its cushioning ability
The result:
➤ Increased friction
➤ Inflammation
➤ Pain and stiffness
Imagine a well-oiled hinge slowly drying out. That’s what happens inside the joint. And without intervention, this process continues to progress
RESTORING WHAT’S LOST: UNDERSTANDING HA INJECTIONS
When the natural hyaluronic acid in the joint starts to break down, one of the most effective ways to address this is through viscosupplementation. In simple terms, viscosupplementation means replenishing the joint with externally supplied hyaluronic acid (HA)—restoring what has been lost over time. These HA injections are designed to:
➤ Replenish synovial fluid
➤ Restore lubrication
➤ Improve joint mechanics
But here’s where things get more nuanced.
Not all HA injections deliver the same results.
WHY ALL HA INJECTIONS DON’T DELIVER THE SAME OUTCOME
It’s easy to think of hyaluronic acid as just “a lubricant.” In reality, its performance depends heavily on how it is designed and formulated.
Today, there are multiple players in the market—ranging from locally available formulations to globally established brands such as Durolane, Synvisc, Hyalgan, Orthovisc, and others. While all of these fall under the category of hyaluronic acid or viscosupplements, they are not identical in how they behave inside the joint.
And this is where the difference begins.
Key factors that influence performance include:
➤ Molecular Weight
Higher molecular weight HA better mimics natural joint fluid, improving cushioning and lubrication
➤ Viscosity
Determines how effectively the joint can absorb load and reduce friction
➤ Source of HA
Non-animal (bacterial-derived) HA is generally preferred due to better safety and lower risk of inflammatory reactions and better biocompatibility
➤ Cross-Linking
Influences how long the HA remains active within the joint
Because of these variations, two HA injections may appear similar on paper— but can perform very differently in clinical practice. The real difference lies not in the brand name alone, but in how effectively the joint environment is restored and sustained over time Among the many HA options available, formulations differ based on how these parameters are balanced—molecular weight, viscosity, cross-linking, and source all influence how the product performs inside the joint. For instance, some formulations are designed for shorter-term lubrication, while others aim for longer residence time through cross-linking. The choice often depends on patient profile, stage of disease, and clinical preference.
ViscoHeal is one such formulation that attempts to balance these factors with a focus on functional joint restoration rather than simple supplementation.
It is available in two variations:
➤ 1% (10 mg/ml) non–cross-linked HA – designed to closely mimic natural synovial fluid behavior
➤ 1.5% (15 mg/ml) cross-linked HA – aimed at providing longer intra-articular residence and sustained effect
Across both, the formulation is built around:
➤ High molecular weight (~3.2 million Dalton)
➤ High viscosity (up to ~400,000 mPas) for improved cushioning
➤ Non-animal (bacterial-derived) source for better safety profile
➤ Preservative-free composition
➤ European-grade API with controlled manufacturing standards
Rather than acting as just a space-filler, such formulations are intended to:
➤ Restore joint lubrication more effectively
➤ Reduce mechanical stress during movement
➤ Support smoother, more stable joint function over time
The goal is not just temporary relief, but a more consistent restoration of joint mechanics, depending on how well these parameters are optimized.
BEYOND LUBRICATION: WHEN MECHANICS ALONE ISN’T ENOUGH
While restoring joint lubrication is a critical first step, especially in early osteoarthritis, it doesn’t always address the full picture.
As the condition progresses, the joint environment becomes more complex—no longer just a mechanical issue, but also:
➤ Inflammatory
➤ Degenerative
➤ Biologically altered
This is where relying on lubrication alone may provide relief, but not always sustained outcomes.
From Alternatives to Allies
Hyaluronic acid (HA) and platelet-rich plasma (PRP) were once viewed as competing options—one mechanical, the other biological.
Today, they are increasingly used together, not as substitutes, but as complementary approaches addressing different aspects of the disease.
➤ Hyaluronic Acid (HA)
Supports joint mechanics by improving lubrication, reducing friction, and enhancing movement
➤ Platelet-Rich Plasma (PRP)
Supports biological activity by influencing inflammation and promoting tissue response
Together, they address both how the joint moves and how the joint responds. Something neither can fully achieve alone.
Why this Combination Matters
Compared to HA alone, combining HA with PRP has been associated with:
➤ Greater reduction in pain scores (VAS)
➤ Improved functional outcomes (WOMAC scores)
➤ Better joint mobility
➤ More sustained clinical response over time
Some studies also suggest enhanced biological activity when both are used together, leading to improved overall outcomes in osteoarthritis management
What This Means for Patients
For patients, this approach shifts the focus from temporary relief to more structured, stage-based care:
➤ Improved pain control
➤ Better joint function and mobility
➤ Potential for longer-lasting outcomes
➤ Reduced reliance on repeated symptomatic treatments
Instead of choosing between options, the goal becomes using them together appropriately for better results.
FINAL THOUGHT
Your knees carry you through life—every step, every movement, every day. And like any system, they need the right environment to function well. Hyaluronic acid may be known for skincare— but in your joints, it’s something far more important:
It’s what keeps you moving. So, whether you’re managing early symptoms or looking to delay progression, understanding the role of HA is the first step toward better joint health. Because real treatment isn’t just about relieving pain— it’s about restoring how the joint works.



